-
AI-Native Platform
Platform
-
Studio
No-code agentic platform delivering the fastest time-to-value and the highest ROI
-
Studio
-
Agentic CRM
CRM
-
Agentic CRM
New era CRM to manage customer & operational workflows
CRM Products -
Agentic CRM
- Industries
- Customers
- Partners
- About
Accelerate Claims Resolution at Scale with Creatio Agentic CRM

Insurance claims processing is still heavily burdened by manual processes, fragmented systems, and slow turnaround times, with claims handlers spending even 40% of their time on administrative tasks rather than on decision-making.
At the same time, expectations are rising. Customers now demand fast, digital, and transparent claims experiences, putting pressure on insurance companies to modernize their operations. This is why claims automation software is rapidly becoming a priority in the insurance industry, with the global market growing from $6.54 billion in 2026 to an estimated $17.09 billion by 2034, driven by the adoption of AI, intelligent automation, and data-driven decisioning.
In this guide, we explore how claims automation works, its key benefits, the role of AI, and how insurers can successfully implement claims automation software in their businesses.
Key Takeaways:
- Insurance claims processing automation streamlines claims management by automating manual data entry, validation, fraud detection, adjudication, and payment processing with minimal human intervention.
- The claims processing system is supported by several automation technologies, such as Robotic Process Automation (RPA), Natural Language Processing (NLP), Optical Character Recognition (OCR), Machine Learning (ML), Artificial Intelligence (AI), and more.
- Automated claims processing enables insurance companies to streamline repetitive tasks, eliminate manual processes, accelerate claims processing, improve claims accuracy and fraud detection, reduce operational costs, and enhance customer experience.
- AI is the core enabler of intelligent claims process automation, improving risk assessment, fraud detection, document processing, and decision-making.
- Manual claims processing is a major bottleneck, but legacy systems, data silos, regulatory requirements, limited flexibility, and high ownership costs can also be challenging when adopting automated systems.
- Creatio enables end-to-end claims automation with no-code tools, intelligent workflow orchestration, and AI agents embedded into processes, helping insurers reduce manual work, improve decision-making, and deliver faster, more transparent claims experiences at scale.
What is Claims Automation?
Claims automation is the process of intake, evaluation, management, and resolution of insurance claims with minimal human involvement, enabled by digital automation technologies such as Robotic Process Automation (RPA), Intelligent Document Processing (IDP), Optical Character Recognition (OCR), and Artificial Intelligence (AI).
Claims automation improves speed, accuracy, and customer satisfaction while maintaining compliance, accuracy, and transparency of traditional claims processing.
How Does Claims Automation Work?
A modern claims processing automation framework typically follows a five-stage lifecycle:
- Intelligent intake - capture claims digitally and structure First Notice of Loss (FNOL) data for processing.
- Data extraction and validation - automatically extract claims data from documents using tools like OCR and IDP, and verify accuracy against policy and system records.
- Fraud and risk assessment - analyze claims using Artificial Intelligence and advanced analytics to detect fraud and assign risk scores.
- Smart adjudication - apply policy rules and AI models to evaluate the claim, and determine coverage, eligibility, and claim value.
- Digital settlement – streamline claims approval, issue payments, and notify customers through automated workflows.
Benefits of Claims Automation in Insurance
Automated claims processing offers multiple benefits, including faster processing, lower costs, improved risk management, and greater customer satisfaction. By digitizing and optimizing each stage of the claims lifecycle, insurers can operate more efficiently while delivering better outcomes for both the business and policyholders.
Faster claims processing
Insurance claims automation solutions significantly accelerate claims processing by eliminating routine steps, such as manual data entry in claim forms, claims routing, document review, and data validation, enabling straight-through processing for low-complexity claims. Manual tasks that once took days can now be completed in minutes, improving responsiveness and throughput.
Improved claims accuracy
Insurance claims processing automation reduces human error by ensuring consistent data capture, validation, and decision-making throughout the entire claims process. By leveraging AI and rule-based logic, insurers can improve the precision of claim assessments, minimize inconsistencies, and ensure decisions are based on complete, verified information. According to McKinsey, insurers that use AI in claims processing saw an average improvement of 3-5% in accuracy.
Operational cost savings
By reducing reliance on manual handling, insurers lower administrative costs associated with claims data entry, document review, and claim handling. Automation also minimizes rework and human errors, further improving operational cost-efficiency.
Improved loss ratios with fraud detection
Advanced AI-powered analytics and fraud detection help identify fraudulent claims early in the process by continuously reviewing patterns and flagging potential issues. This reduces fraudulent payouts, directly improving loss ratios and overall underwriting profitability.
Strengthen customer loyalty
Faster claim resolution, transparent communication, and seamless digital experiences enhance customer satisfaction. With AI-powered chatbots, customers can receive answers to their inquiries 24/7 and easily check their claim statuses themselves. A smooth claims process and improved customer service strengthen trust and increase policyholder retention and lifetime value.
Greater scalability
With claims automation solutions, insurers can process an increasing amount of claims during high-demand periods without growing headcount or overloading operations, ensuring consistent performance and service quality even during peak volumes.
The Role of AI in Claims Automation
Artificial intelligence is at the core of modern claims automation, enabling insurers to move beyond simple rule-based processing toward intelligent, adaptive, and predictive claims operations. AI enhances the entire claims process by improving decision-making, reducing manual effort, and enabling real-time insights with minimal human oversight.
Today, insurers leverage a range of AI capabilities to automate and optimize claims processing:
- Machine Learning (ML) - identifies patterns in historical claims data to support risk scoring, fraud detection, and decision-making.
- Natural Language Processing (NLP) - extracts relevant data from structured and unstructured data such as emails, reports, and customer communications.
- Computer Vision - analyzes images and videos (e.g., vehicle damage, property loss) for automated damage assessment.
- Intelligent Document Processing (IDP) - combines OCR and AI to extract and validate data from documents.
- Predictive Analytics - forecasts claim outcomes, severity, repair estimates, likelihood of fraud, etc.
- Conversational AI - powers chatbots and virtual assistants for FNOL intake and customer communication.
These technologies enable faster, more accurate, and scalable claims handling, especially for high-volume, low-complexity claims. According to a McKinsey report, AI can also improve outcomes in more complex claims. Based on UK insurer Aviva’s case study, the AI helped cut liability assessment time by 23 days, improve case routing by 30%, and reduce customer complaints by 65%, ultimately saving the company over $82 million in 2024.
The future of AI in insurance claims automation
Looking ahead, AI is expected to play an even more significant role in streamlining claims processing and enabling more proactive claims management. Advances such as generative AI, predictive AI, and AI copilots are already supporting claims professionals by automating repetitive tasks, summarizing case information, recommending next steps, and handling routine communication.
The next step in AI evolution is autonomous agents, which can independently execute tasks within predefined workflows, such as validating data, triaging claims, or triggering actions, while continuously learning from outcomes. As these capabilities evolve, insurers will be able to streamline increasingly complex claims with minimal manual intervention.
However, despite these advancements, AI is not a replacement for human expertise. Instead, it reshapes the role of claims professionals. Intelligent automation takes over repetitive, data-intensive tasks, allowing claims adjusters and handlers to focus on higher-value activities such as complex case evaluation, customer interaction, and exception handling.
Humans increasingly act in an oversight capacity, reviewing AI-generated insights, validating outcomes, and ensuring decisions align with business rules, regulatory requirements, and ethical standards. Crucially, the final decision remains in human hands.
Essential Features of Insurance Claims Automation Software
To deliver real value, claims automation tools must go beyond basic workflow automation and provide capabilities that support the typical insurance claims lifecycle.
The most effective platforms offer these key features:
Integrated claims lifecycle management
Automate the entire insurance claims lifecycle with structured, end-to-end digital workflows that support review, investigation, and resolution. Claims are automatically routed, progressed, and tracked across teams, ensuring consistent execution, reduced delays, and full visibility at every stage.
FNOL (First Notification of Loss)
Enables digital First Notice of Loss submission across multiple channels, including web, mobile, chatbots, and APIs, ensuring claims are submitted accurately from the outset.
Auto-sorting (smart triage)
Automatically classifies and routes claims based on predefined rules and AI-driven insights. Low-risk, straightforward claims can be processed automatically with minimal human involvement, while complex or high-risk cases are directed to the appropriate specialists.
Claims investigation
Collects and consolidates customer and relevant data from multiple sources, such as digital channels, call transcripts, third-party reports, medical records, and external databases, into a unified view. This enables more efficient investigations, improves fraud detection, and ensures greater transparency throughout the process.
Claims adjustment and appraisal
Digitize claims adjustment workflows and standardize appraisal processes to ensure consistent, transparent, and personalized claim handling. Claims automation software equips field agents with mobile tools to assess damages, capture data on-site, and make faster, more informed decisions aligned with company best practices.
Instant status updates
Provide real-time visibility into claim status for both internal teams and customers. Automated notifications and AI-powered chatbots improve transparency, reduce inbound inquiries, and enhance the overall customer experience by keeping stakeholders informed at every stage of the process.
Reporting and analytics
Insurance claims automation platforms offer visibility into claims performance with built-in reporting and analytics tools. AI-powered tools analyze trends across common claim types, processing timeframes, costs, and more to provide insights into operational efficiency.
Key Challenges in Insurance Claims Automation
While insurance claims process automation offers significant benefits, insurers can encounter a range of challenges when implementing and scaling these solutions. These obstacles can limit efficiency gains, increase costs, and slow down transformation efforts if not addressed strategically.
- Data fragmentation and legacy systems constraints - claims data is often spread across multiple legacy systems and formats, making it difficult to unify, process, and maintain consistency throughout the lifecycle. To remedy this, implement a unified data model and integrate systems through a centralized platform, middleware, or APIs to ensure consistent, real-time data access.
- Regulatory compliance and data security requirements - insurance companies must meet strict regulatory standards for data security, privacy, and governance while maintaining full auditability and customer trust. To avoid issues, choose a platform that supports built-in compliance, data protection, and governance controls.
- High total cost of ownership - implementing and maintaining automation solutions, especially legacy or heavily customized systems, can lead to high upfront and ongoing costs. Choose a no-code platform that reduces development, maintenance, and infrastructure costs.
- Lack of flexibility - many insurers rely on rigid systems that are difficult to modify or integrate, limiting flexibility and slowing down innovation and scalability. Implement a solution that offers a composable architecture that enables modular upgrades, easy customization, and seamless integration with existing and future systems.
Ultimately, many of these challenges can be effectively addressed by selecting the right claims automation platform. An agentic no-code platform like Creatio helps insurers overcome data fragmentation, reduce costs, and adapt quickly to changing business and regulatory demands.
With its no-code capabilities, composable architecture, and AI-powered automation, Creatio enables organizations to unify data, streamline workflows, and continuously optimize claims operations without a heavy reliance on IT.
How to Get Started with Insurance Claims Automation
Implementing claims automation requires a structured approach that aligns technology with business goals, operational processes, and customer expectations. Insurers should not only adopt the technology effectively but also optimize processes and prepare their employees for the change.
The following five steps provide a practical roadmap to begin the automation journey:
1. Perform a strategic audit
The first step is to assess the current claims processes, systems, pain points, and manual tasks. A strategic audit helps identify inefficiencies, bottlenecks, and opportunities for automation, while also defining clear business objectives and expected outcomes.
2. Prioritize workflows
Not all processes should be automated at once. Insurers should identify and prioritize high-impact workflows, typically those that are repetitive, high-volume, and rule-based, that heavily rely on manual work. Starting with these areas allows organizations to achieve quick wins, demonstrate value, and build momentum for broader automation initiatives.
3. Select the right insurance claims automation platform
Choosing the right claims system is critical. The selected platform should support end-to-end claims automation in a centralized system, be flexible enough to be customized to unique needs, and integrate easily with existing systems. It should also include built-in AI capabilities, scalability, and compliance features to support long-term growth.
4. Implement the system and train your team
Successful implementation of automated claims processing tools requires careful planning, including system configuration, integration, and testing. Choose a vendor with a reliable partner community to support fast and painless implementation.
Equally important is preparing teams for change through training, clear communication, and change management. Employees need to understand how to work alongside automation tools and how their roles will evolve in the new environment.
5. Track KPIs consistently
Insuring companies should track key performance indicators such as cycle time, cost per claim, fraud detection rates, and customer satisfaction to measure success. Ongoing analysis enables insurers to refine processes, optimize performance, and maximize the return on investment.
Insurance Claims Automation with Creatio
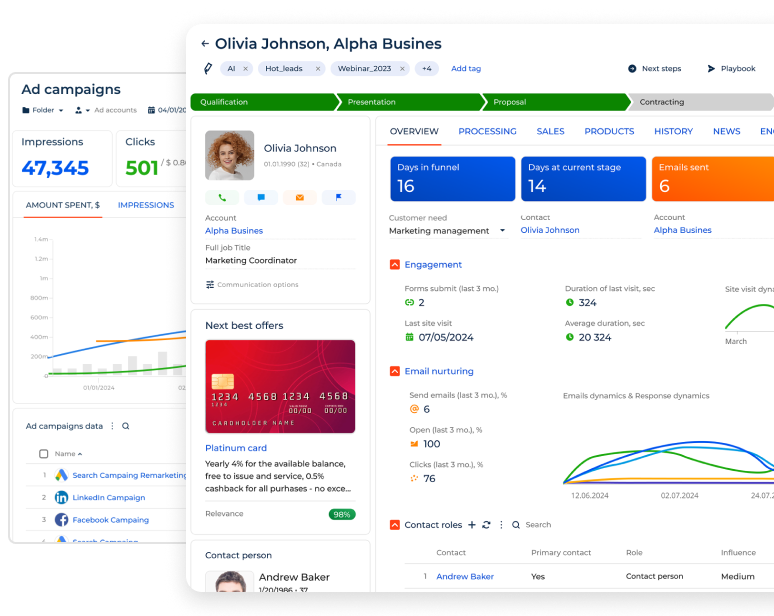
Creatio enables insurers to automate end-to-end insurance claims processes on an agentic CRM and workflow platform that has no-code and AI at its core. With intelligent workflow automation, unified data, and powerful AI agents, Creatio insurance CRM empowers organizations to accelerate claims processing, reduce operational costs, improve accuracy, and deliver transparent experiences to policyholders, all while maintaining full control and compliance.
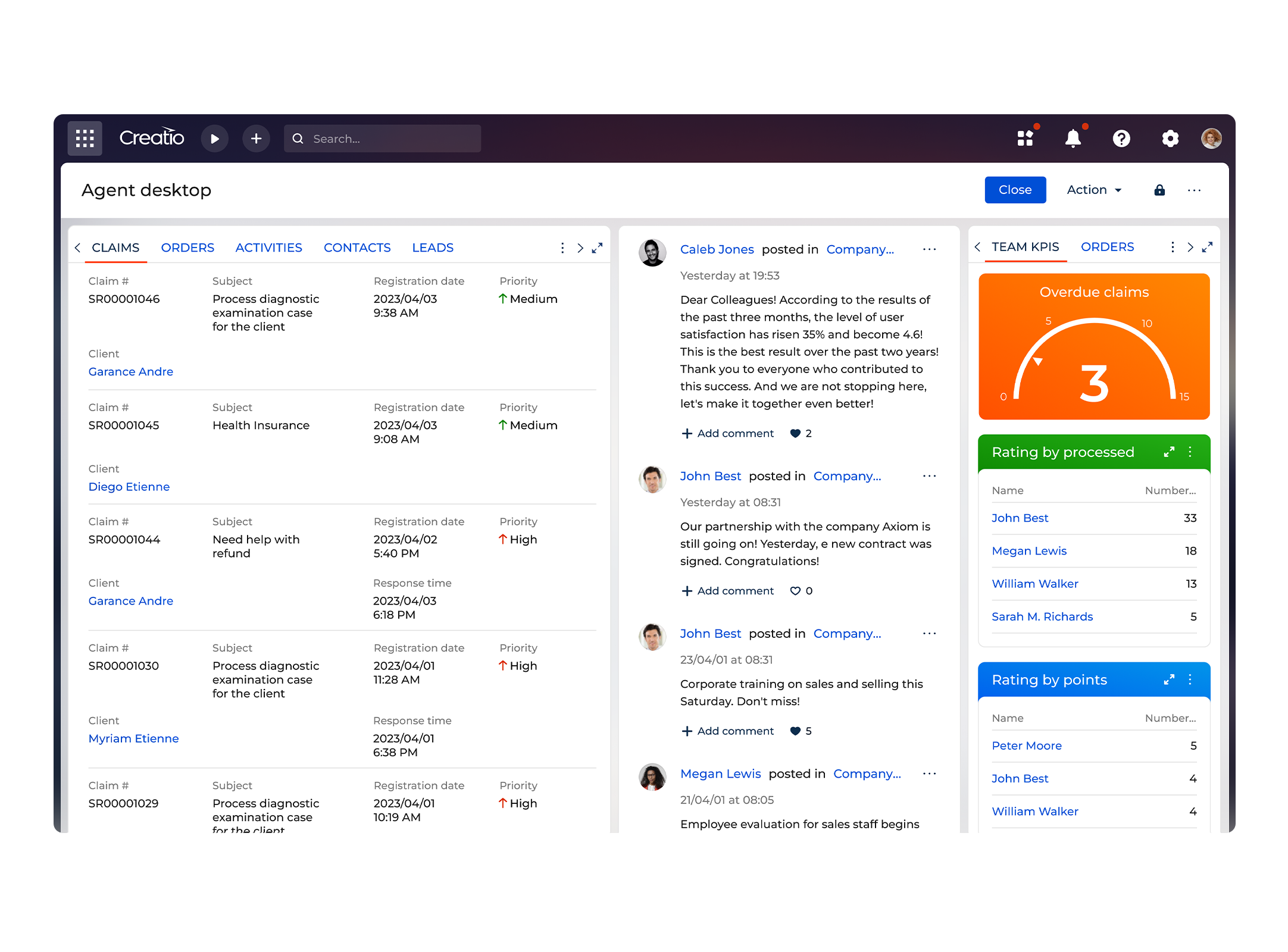
With Creatio CRM, insurers can digitize the entire claims lifecycle, from FNOL to settlement, within a single AI-native platform. Claims are captured through digital channels, automatically routed, validated, and processed using configurable workflows. This reduces manual handling and ensures consistency across all claim types.
A key capability is the use of AI agents embedded directly into claims workflows. These agents can:
- Automatically review incoming claims and check for missing or inconsistent data
- Validate information against policies and external data sources
- Route claims to the right adjuster or trigger straight-through processing
- Flag potential fraud or high-risk cases
- Determine coverage, eligibility, and claim value
- Generate summaries and assist adjusters with next steps
- Support effective decision-making with data-driven insights
Importantly, Creatio CRM keeps a human-in-the-loop approach. While AI agents automate routine tasks with minimal human intervention, claims professionals retain control over approvals and final decisions, ensuring accuracy, compliance, and trust.
Case Study: Heritage Life Insurance Company
Find out how Heritage Life Insurance Company decreased claims processing times and lowered interest payments with Creatio insurance CRM
Creatio’s agentic no-code platform and composable architecture allow insurers to quickly configure claims processes, decision rules, and integrations without heavy IT involvement. This makes it easy to adapt workflows as business needs, regulations, or products change. In addition, Creatio supports seamless integration with existing systems, such as policy administration, billing, and external data providers, so insurers can modernize claims automation without replacing their core infrastructure.
Creatio CRM also provides real-time visibility into claims operations. Teams can track claim status, workloads, and performance metrics in one place, enabling faster decisions and better coordination across departments.
Summary
As claims volumes grow and customer expectations shift toward faster, more transparent service, insurers can no longer rely on manual, fragmented processes. Claims processing automation with technologies such as Robotic Process Automation (RPA), Natural Language Processing (NLP), and AI has become essential for improving efficiency, reducing costs, and enhancing accuracy and fraud detection.
Platforms like Creatio provide the flexibility, intelligence, and scalability needed to modernize claims operations end-to-end. With no-code tools, composable architecture, and AI agents embedded into insurance claims processing workflows, insurers can not only keep up with demand and maintain a competitive advantage but also build a future-ready, efficient, and customer-centric claims operation.